Background
Asymmetry of motor signs is a cardinal feature of Parkinson disease which may impact phenotypic expression.
Objective
To investigate the relationship between lateralization of motor signs and symptom progression and severity during longitudinal observation for up to 4 years in a naturalistic study.
Methods
We analyzed data prospectively collected during the NINDS Parkinson Disease Biomarker Project (PDBP). We defined the Movement Disorder Society Revision of the Unified Parkinson Disease Rating Scale (MDS-UPDRS) part II as the primary measure of symptom progression. Left side predominant subjects were those whose lateralized motor scores on the MDS-UPDRS part III were ≥2 points higher on the left side than on the right side of the body. Multiple regression models (controlled for age, gender, education years, ethnicity, levodopa equivalent daily dose (LEDD) at baseline, and years with PD) were used to estimate the rate of symptom progression comparing left predominant (LPD) with non-left predominant (NLPD) subjects. A sensitivity analysis was performed using the same multiple regression models in the subgroups of low (0–26) or high (>27) MDS-UPDRS II score at baseline to determine if PD severity influenced the results.
Results
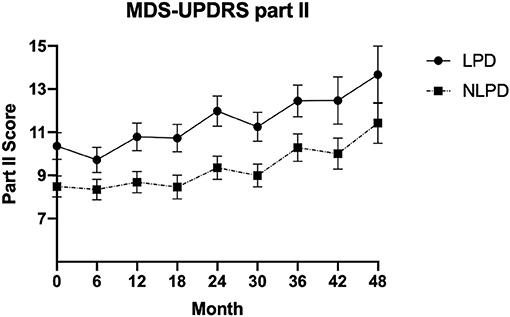
We included 390 participants, 177 LPD and 213 NLPD. We found that MDS-UPDRS part II progression from baseline to 48 months was faster in LPD compared to NLPD (0.6 points per year faster in LPD, p = 0.05). Additionally, the LPD group was statistically significantly worse at baseline and at 48 months in several subparts of the MDS-UPDRS and the Parkinson's Disease Questionnaire-39 (PDQ-39) mobility score. Significantly slower progression (difference of −0.8, p = 0.01) and lower score at 48 months (difference of −3.8, p = 0.003) was seen for NLPD vs. LPD in the group with lower baseline MDS-UPDRS part II score.
Conclusion
Left side lateralization was associated with faster symptom progression and worse outcomes in multiple clinical domains in our cohort. Clinicians should consider using motor predominance in their counseling regarding prognosis.